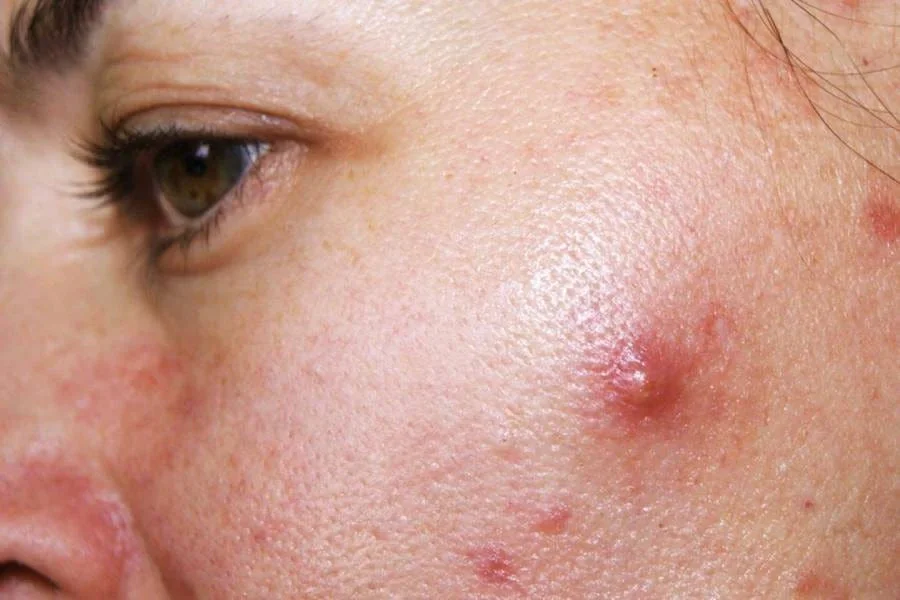
Post-acne syndrome refers to a group of symptoms that some people report after completing treatment for acne, especially after medications such as isotretinoin. These symptoms may include skin changes, hormonal concerns, fatigue, or mood changes, although research has not identified a single medical condition that explains all cases.
Current medical evidence shows that many symptoms discussed under the label post-acne syndrome require individual evaluation because several health factors can produce similar effects. Scientists continue to study possible biological mechanisms, including inflammation, hormone signaling, and nervous system responses.
Understanding these possibilities helps patients interpret symptoms and seek appropriate medical assessment when needed.
Key Takeaways
- Post-acne syndrome is a term used to describe symptoms that some people report after acne treatment, but it is not currently recognized as a formal medical diagnosis in dermatology.
- Symptoms discussed under post-acne syndrome may include skin dryness, hormonal concerns, fatigue, or mood changes, although these symptoms can have multiple medical causes.
- Severe inflammatory acne and its treatments can lead to long-term skin effects, such as acne scarring, dark spots, and post-inflammatory hyperpigmentation, especially in darker skin tones.
- Current medical research has not confirmed a single biological cause for post-acne syndrome, and many reported symptoms require individual medical evaluation.
- Doctors usually assess persistent symptoms by reviewing medical history, evaluating possible underlying conditions, and recommending treatment based on the specific issue rather than the label alone.
What Is Post-Acne Syndrome
Definition Of Post-Acne Syndrome
Post-acne syndrome is a term used to describe symptoms that some people report after completing treatment for acne, particularly after medications such as isotretinoin. The phrase does not refer to a formally recognized medical diagnosis. Instead, it serves as a descriptive label for ongoing symptoms that patients associate with past acne treatment.
These reported symptoms may include skin dryness, fatigue, mood changes, hormonal concerns, or other physical complaints. Research continues to study whether these symptoms share a common biological cause. In many cases, doctors evaluate each symptom individually to determine the most likely medical explanation.
Post-Acne Withdrawal Syndrome Explained
Some articles use the phrase post-acne withdrawal syndrome to describe similar symptoms. The term suggests that the body reacts after stopping acne medication. Researchers continue to examine whether these symptoms relate to medication effects or other medical conditions.
Doctors usually focus on the specific symptoms rather than the label. Careful medical evaluation helps identify possible causes. This approach improves treatment planning and avoids confusion.
Post-Acne Syndrome Symptoms
Sexual And Hormonal Symptoms
Some reports linked to post-acne syndrome mention hormonal or sexual health symptoms, which researchers continue to examine in discussions about Accutane erectile dysfunction recovery. These may include fatigue, reduced libido, or hormone changes. Researchers study whether acne medications can influence hormone signaling in the body.
Doctors usually review hormone levels and medical history during evaluation. Many factors can affect hormones, including stress, illness, or other medications. A full clinical review helps determine the likely cause.
Neurological And Cognitive Symptoms
Some patients report changes in mood, focus, or memory after acne treatment. These symptoms are sometimes discussed in research on isotretinoin. Scientists study whether the medication interacts with brain signaling pathways.
Mental health can change for many reasons. Severe acne itself may affect emotional health and self-image. When acne improves, mood often improves as well. Doctors assess mental health history and lifestyle factors when reviewing these concerns.
Gastrointestinal Symptoms
Digestive symptoms are also reported in some discussions about post-acne syndrome. These may include stomach discomfort or changes in digestion. Research has explored whether gut inflammation could play a role.
Evidence remains limited. Many digestive symptoms come from common conditions such as food intolerance or stress. Doctors often review diet, medication history, and digestive health before drawing conclusions.
Skin And Dryness Symptoms
Skin dryness is one of the most common side effects of acne medication. Retinoids reduce oil production in the skin. This change helps treat acne but can cause dry lips and dry skin during treatment.
Some people notice dryness for a short time after treatment ends. Good skin care can help restore the skin barrier. Moisturizers and gentle cleansers often reduce irritation.
Other skin concerns may appear after acne heals. These include acne scarring, dark spots, and uneven skin tone. Dermatologists call these pigment changes post inflammatory hyperpigmentation PIH. They appear more often in darker skin tones.
Acne And Isotretinoin: How They Affect The Body
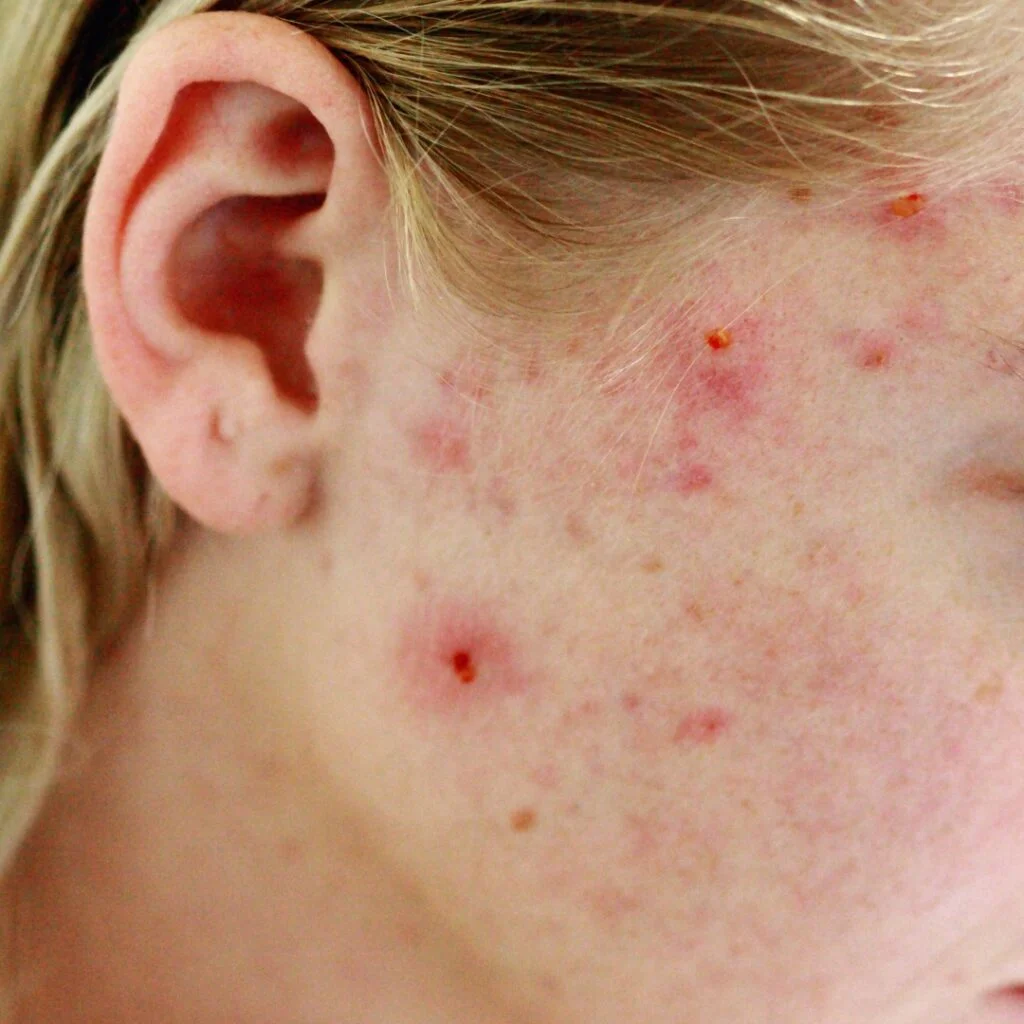
What Is Inflammatory Acne
Inflammatory acne develops when oil glands produce too much sebum. Bacteria grow in blocked pores and trigger the immune system. This reaction causes redness, swelling, and painful bumps.
Dermatologists classify several types of acne. These include papules, pustules, nodules, and cysts. Inflammatory acne often requires medical treatment to prevent scarring.
How Isotretinoin Works On Sebaceous Glands
Isotretinoin treats severe acne by shrinking oil glands in the skin, a medication often known by the brand name Accutane. Lower oil levels reduce bacterial growth and clogged pores. The medicine also improves the shedding of skin cells within hair follicles.
Board-certified dermatology
Skip the waiting room. See a dermatologist today.
Get expert skin care from a licensed derm – no referral needed, no commute required.
These effects make isotretinoin one of the most effective treatments for severe acne. Doctors monitor patients closely during treatment. Most side effects improve after therapy stops.
Why Some Acne Does Not Go Away
Acne may continue even after treatment for several reasons. Hormones can stimulate oil production in the skin. Genetics also influence how skin responds to inflammation.
Different skin types respond differently to acne. Some people develop more inflammation and pigment changes. Others may experience repeated breakouts.
Long-Term Effects Of Severe Acne
Severe acne can cause lasting skin changes. One common result is acne scarring. Deep inflammation damages skin tissue, leading to uneven texture.
Another effect is pigment change. After acne heals, the skin may produce extra pigment. This process creates dark marks called post-inflammatory hyperpigmentation PIH. Sun protection often helps prevent these spots from getting darker.
Causes And Scientific Debate
Biological Mechanisms Proposed In Research
Researchers have suggested several possible causes for symptoms linked to post-acne syndrome. Some studies examine how retinoids affect gene activity in cells. These changes may influence inflammation or tissue repair.
Scientists also study hormone signaling and immune responses. These systems regulate many body functions. However, research has not confirmed a single mechanism that explains all reported symptoms.
Why Evidence On Post-Acne Syndrome Is Limited
Scientific evidence remains limited because many reports rely on surveys or case studies, a pattern also noted in research on Accutane’s long-term effects. These reports help researchers notice patterns. However, they cannot prove a direct cause-and-effect relationship.
Large clinical studies are needed to confirm links between symptoms and acne treatment. Until more research is available, doctors interpret each case carefully. Individual evaluation remains important.
How Doctors Evaluate Persistent Symptoms
Medical History And Symptom Timeline
Doctors begin with a detailed medical history. They review acne treatments, medications, and the timing of symptoms. Knowing when symptoms started helps identify possible triggers.
Doctors may also ask about diet, sleep, and stress. These factors influence inflammation and overall health. Blood tests may help evaluate hormone levels or other medical conditions.
Conditions That May Mimic Post-Acne Syndrome
Some symptoms attributed to post-acne syndrome may have other causes. Persistent redness, for example, may relate to red skin syndrome or topical steroid addiction. Both conditions affect blood vessels in the skin.
Other symptoms may come from hormonal imbalance or digestive conditions. Doctors evaluate these possibilities during diagnosis. This process ensures that treatment focuses on the correct condition.
ACNES Syndrome And Related Conditions
What Is ACNES Syndrome
ACNES syndrome stands for abdominal cutaneous nerve entrapment syndrome. It occurs when small nerves in the abdominal wall become compressed. This pressure causes localized pain.
The condition affects nerves rather than the skin itself. It is unrelated to acne or acne treatment.
ACNES Syndrome Symptoms
Common ACNES symptoms include sharp or burning pain in a small area of the abdomen. The pain may increase when the skin is pressed. Movement or stretching may also worsen the discomfort.
Doctors diagnose the condition through physical examination and nerve testing.
Abdominal Cutaneous Nerve Entrapment Syndrome
The full name of abdominal cutaneous nerve entrapment syndrome describes the cause of the pain. Nerves that provide sensation to the abdominal skin become trapped between muscle layers.
This compression disrupts nerve signals. It leads to localized pain and tenderness.
ACNES Treatment Options
Doctors treat ACNES with several methods. Local anesthetic injections can reduce nerve irritation and confirm the diagnosis. Physical therapy may also help relieve pressure on the nerve.
In rare cases, surgery may be required to release the trapped nerve.
Can ACNES Syndrome Go Away
Many patients improve with treatment. Pain may decrease after injections or physical therapy. Doctors monitor symptoms to determine whether further treatment is needed.
Treatment And Management Approaches
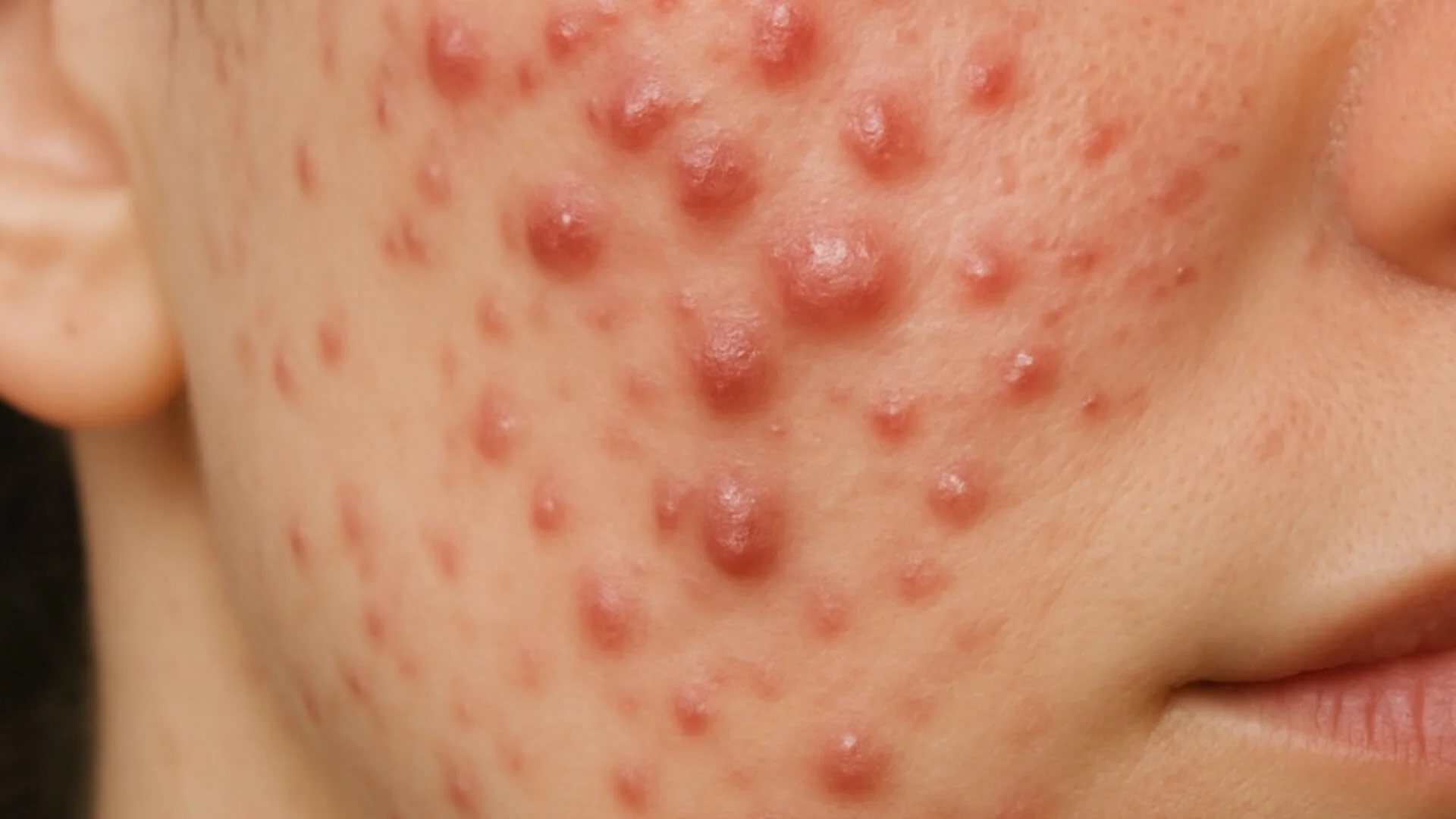
Symptom-Based Treatment
Treatment depends on the specific symptoms identified. Dermatologists may recommend gentle skin care to repair the skin barrier. Anti-inflammatory products may help calm irritated skin and reduce inflammation.
For pigment changes or scarring, doctors may suggest chemical peels or other dermatology procedures. These treatments improve skin texture and help fade dark spots.
Hormonal And Mental Health Evaluation
Doctors may also evaluate hormone levels when fatigue or hormonal symptoms appear. An endocrinologist may assist when a hormone imbalance is suspected.
A mental health evaluation may help when mood changes occur. Dermatologists often work with other specialists to provide complete care.
DermOnDemand explains these options through educational resources rather than promoting treatments. Clear medical information helps patients understand realistic expectations.
Common Misconceptions About Post-Acne Syndrome
Is Post-Acne Syndrome A Recognized Diagnosis
The term post-acne syndrome is widely discussed online. However, it is not a formal diagnosis in dermatology guidelines. Doctors usually focus on individual symptoms rather than a single label.
Understanding this difference helps avoid confusion. Multiple health conditions can cause similar symptoms.
Does Isotretinoin Always Cause Post-Acne Syndrome
Isotretinoin remains one of the most studied acne medications. Many patients complete treatment without long-term complications. Some reports describe persistent symptoms, but research has not proven a consistent cause.
Doctors discuss possible risks before treatment begins. Monitoring during therapy helps detect side effects early.
When Medical Evaluation Is Recommended
Symptoms That Should Be Reviewed
Ongoing symptoms after acne treatment can raise understandable questions about their cause. Persistent fatigue, unexplained pain, mood changes, or skin concerns that do not improve may warrant medical review. Early evaluation allows a doctor to examine your symptoms, consider possible causes, and recommend appropriate next steps based on your health history.
If symptoms continue or begin to interfere with daily life, a dermatology consultation can help clarify what is happening and whether further evaluation is needed.