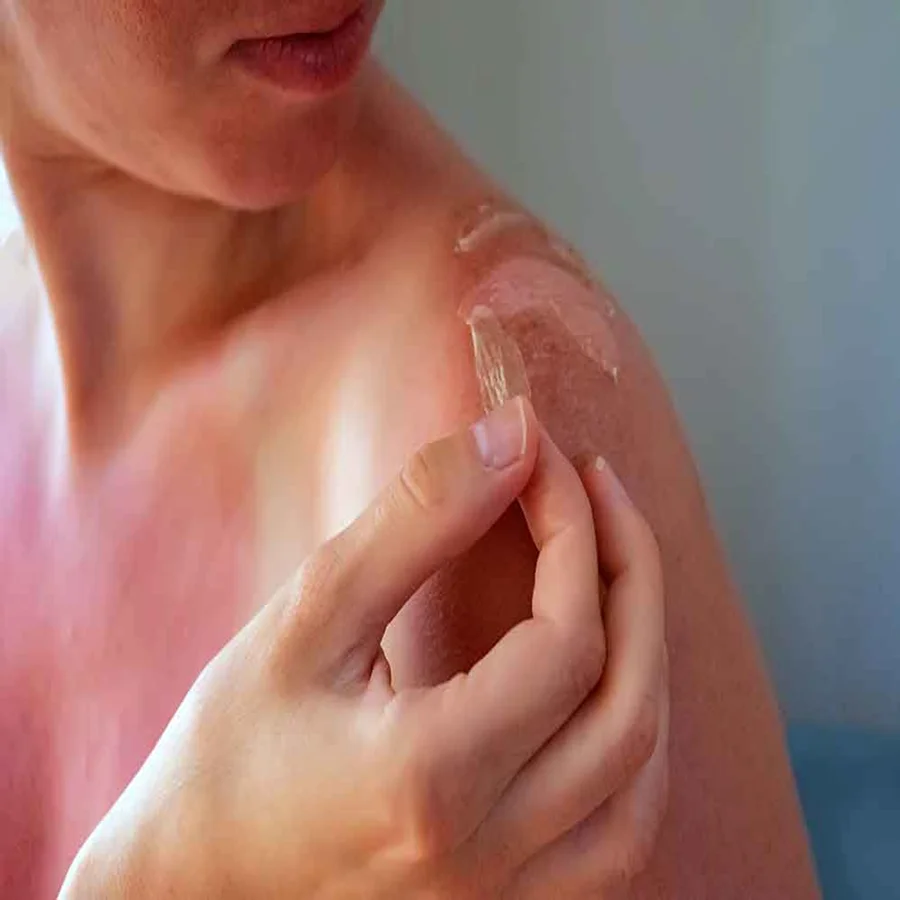
Yes, high cholesterol and Accutane can be related. Isotretinoin, the drug often called Accutane, can raise triglycerides and sometimes total or LDL cholesterol during treatment. These lipid changes are common and are tracked with blood tests reported in mg/dL.
DermOnDemand shares educational information about these effects, and dermatologist Dr. Alicia Atkins explains that doctors monitor lipid levels during therapy to ensure treatment remains safe.
Key Takeaways
- Isotretinoin (Accutane) can raise cholesterol and triglyceride levels in some people because it alters how the liver processes fats.
- Lipid changes often appear within the first 1 to 2 months of treatment. Doctors use blood tests to monitor cholesterol and triglyceride levels during this time.
- Doctors review the full lipid panel – total cholesterol, LDL, HDL, and triglycerides – to determine whether the change is mild or requires care.
- In most patients, cholesterol levels return to normal after treatment ends because the drug’s effects fade with time.
Does Accutane Raise Cholesterol?
Yes, Accutane can increase cholesterol in some patients. Accutane is another name for isotretinoin, a medicine doctors prescribe to treat severe acne vulgaris.
The medicine works by reducing oil in the skin. This helps control acne vulgaris breakouts. At the same time, it can affect how the body handles fats in the blood.
Cholesterol and triglycerides are fats that move through the blood. Some patients see higher levels during isotretinoin therapy. Doctors track these changes with blood tests.
For most people, the increase is small. Levels often return to normal after treatment ends.
Why Accutane Raises Cholesterol and Triglycerides?
Isotretinoin can change how the body handles fats. The medicine affects how the liver processes lipids. This may increase cholesterol or triglyceride levels during treatment.
Researchers have studied high cholesterol and Accutane for many years, including research into Accutane’s mechanism of action and its effects on lipid metabolism. Studies show the medicine can change how the liver manages fats in the blood, including increases in triglycerides that doctors monitor during treatment, as explained in Accutane and triglycerides.
Because of this, doctors monitor lipid levels during therapy. These changes do not mean the medicine is unsafe. They show why regular medical checks are important.
How Isotretinoin Affects Lipid Metabolism
The liver helps control cholesterol and triglyceride levels in the blood. Isotretinoin can change how the liver processes fats by affecting enzymes that regulate lipid production and breakdown. This can lead to elevated triglycerides and, sometimes, elevated cholesterol during treatment, which is why doctors also monitor liver health and possible concerns such as Accutane liver damage years later.
The medication may also slow the removal of triglycerides from the bloodstream. When this happens, fats can stay in the blood longer than usual. As a result, lipid levels on a blood test may increase.
These changes are often temporary and improve after treatment ends. Doctors monitor them with lipid panel tests during therapy. Most patients do not notice symptoms when lipid levels rise slightly.
Cholesterol and Triglycerides on Accutane
Doctors measure cholesterol and triglycerides with a lipid panel test. This test is done before and during isotretinoin therapy. It helps doctors see how the body responds to the drug.
Small increases are common. Many patients see levels return to normal after treatment ends. Doctors watch results over time to see if levels stay stable.
DermOnDemand’s educational information explains that most lipid changes are manageable when monitored by doctors.
Understanding Lipid Panel Results
A lipid panel checks markers used to evaluate heart health. These markers include total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides.
Doctors also review HDL levels because HDL helps remove extra cholesterol from the blood. Healthy HDL levels help balance other lipids in the body.
Triglycerides store energy in fat cells and move through the bloodstream. Doctors study all lipid markers together to understand a patient’s health.
How Common Lipid Changes Are
Lipid changes are a known side effect of isotretinoin treatment. Studies show that about 1 in 3 patients develop higher triglyceride levels during therapy. Cholesterol increases occur in roughly 1 in 10 patients.
In most cases, the change is mild. Blood test results may rise slightly above the normal range but usually stay within levels doctors consider safe.
Because these changes can occur, dermatologists monitor lipid levels with regular blood tests. If triglyceride or cholesterol levels rise too high, doctors may adjust the dose or repeat testing.
When Lipid Levels Become Concerning
Doctors become more concerned when triglycerides or cholesterol levels rise well above normal.
Triglyceride levels above 300 mg/dL usually lead doctors to repeat testing and recommend diet or lifestyle changes. When triglycerides reach 500 mg/dL or higher, the risk of pancreatitis increases. At that point, doctors may lower the isotretinoin dose or stop treatment.
Total cholesterol can also increase during therapy. Levels above 300 mg/dL may require closer monitoring or treatment adjustments.
Doctors review cholesterol and triglyceride results using medical guidelines. If levels rise too much, doctors may change the treatment plan.
Who Should Be Careful With Accutane
Isotretinoin can effectively treat severe acne, but some patients need closer monitoring. Certain health conditions increase the chance of lipid changes.
Doctors review medical history before prescribing isotretinoin. They consider family history, cholesterol levels, and metabolic health.
DermOnDemand educational guidance explains that treatment plans depend on each patient’s health.
Can You Take Accutane With High Cholesterol?
Some patients start treatment with higher cholesterol levels. In many cases, isotretinoin can still be used with careful monitoring.
Some conditions increase the risk of lipid changes. These include inherited lipid disorders, obesity, and metabolic syndrome.
Doctors review how high the cholesterol level is and whether other risk factors exist. They may suggest lifestyle changes during treatment.
Cholesterol Monitoring During Accutane Treatment
Blood tests are an important part of isotretinoin therapy. Doctors use lipid panels to check cholesterol and triglycerides.
Regular testing helps detect changes early. Doctors review results together with the patient’s health history.
Board-certified dermatology
Skip the waiting room. See a dermatologist today.
Get expert skin care from a licensed derm – no referral needed, no commute required.
Clinical Monitoring Guidelines
Doctors follow standard monitoring steps during isotretinoin therapy. These include baseline tests and follow-up blood work.
Testing schedules may change based on patient risk factors. Doctors interpret results in light of the patient’s medical history.
Blood Tests Before Starting Treatment
Doctors often order blood tests before starting isotretinoin. These tests measure cholesterol, triglycerides, and other markers.
Baseline results help doctors compare future tests and detect changes.
How Often Are Lipid Tests Done?
Doctors usually check lipid levels before starting isotretinoin treatment. Another test is often done about 4 to 8 weeks after treatment begins, when lipid changes most commonly appear.
If results remain stable, additional tests may be done later in treatment or when the dose changes.
When Triglycerides May Require Stopping Accutane
Doctors monitor triglyceride levels during isotretinoin treatment because very high levels can increase the risk of pancreatitis.
These decisions depend on the patient’s overall health and how quickly triglyceride levels increase during treatment.
Managing High Cholesterol During Accutane
If lipid levels rise during treatment, doctors may suggest ways to manage them. These steps help keep cholesterol and triglycerides within safe ranges.
How to Lower Cholesterol While on Accutane
Doctors often suggest simple habits that support healthy lipid levels.
These may include:
- Eating a balanced diet with less saturated fat
- Regular exercise
- Keeping a healthy weight
These habits help support heart health during therapy.
Dose Adjustments or Medication
If lipid levels rise too much, doctors may lower the isotretinoin dose. Lower doses can reduce lipid changes.
In some cases, doctors may prescribe medicines that help control cholesterol.
After Treatment: Cholesterol Recovery
In most cases, cholesterol and triglyceride levels return to normal after the treatment. Doctors may repeat blood tests after treatment to confirm recovery.
Temporary Nature of Most Lipid Changes
Most lipid changes from isotretinoin are temporary, although patients often ask about possible long-term effects of Accutane after treatment. Cholesterol and triglyceride levels usually return to baseline once treatment ends.
Doctors may repeat tests to confirm that lipid levels have normalized.
Does Cholesterol Go Down After Stopping Accutane?
For most patients, cholesterol levels drop after therapy ends. The liver slowly returns to normal function once the medicine leaves the body.
Accutane and Cholesterol Long-Term Effects
Long-term changes in cholesterol from isotretinoin are rare. Research shows lipid increases during treatment are usually temporary.
DermOnDemand educational materials explain that learning about potential side effects, including changes in cholesterol levels, helps patients understand their treatment and make informed health decisions.
If you want to discuss acne treatment options or isotretinoin therapy with a dermatologist, you can start treatment with DermOnDemand online.