Key Takeaways
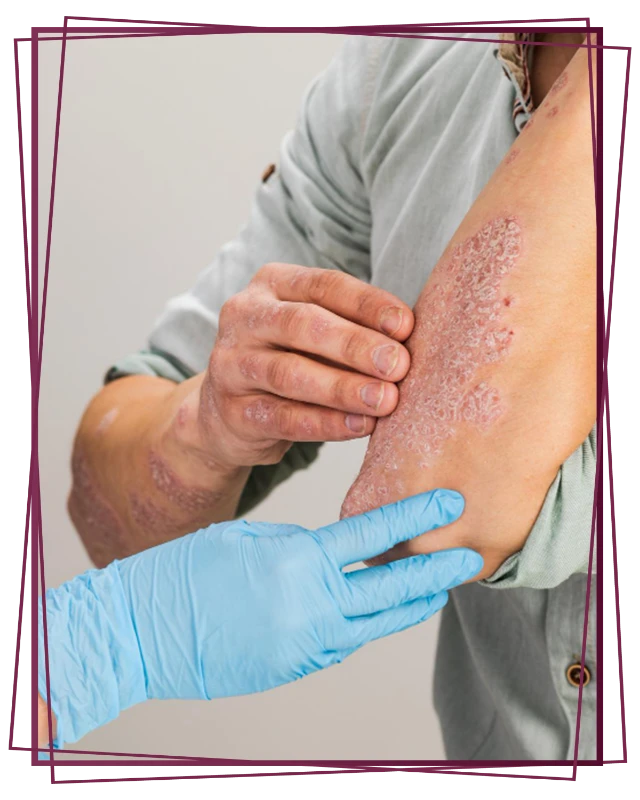
- Accutane can cause severe skin dryness and irritation, and the resulting barrier damage can lead to eczema-like rashes or worsen existing eczema.
- Not every rash on isotretinoin is true eczema, so it is important to distinguish simple dryness and retinoid dermatitis from more persistent inflammatory skin changes.
- Basic care often starts with gentle skincare, daily moisturizing, lip balm, and avoiding triggers such as harsh cleansers, friction, and excessive sun exposure.
- Hand rashes are common during isotretinoin therapy because frequent washing, soap, and daily friction can make already dry skin more inflamed.
- A dermatologist should be consulted for symptoms such as deep cracks, blistering, severe itching, signs of infection, or a rash that does not improve with simple home care.
Can Accutane Cause Eczema?
Accutane can trigger eczema-like symptoms in some people, though it does not mean every rash during isotretinoin therapy is true eczema. This pattern overlaps with other skin rashes linked to Accutane, which is why the exact appearance and timing of symptoms matter. The drug reduces oil production, which can weaken the skin barrier over time.
When the barrier is less effective, dry skin, itching, and inflammation become more likely. People with a history of eczema or other skin conditions may notice that common side effects feel stronger.
Why Skin Gets Dry and Inflamed
The effects of isotretinoin begin with a significant reduction in sebum, the natural oil that helps protect the skin’s surface. Less oil production often leads to tightness, flaking, dry lips, and skin irritation on the face, hands, and arms.
Once the barrier is dry, the skin loses water more easily and becomes more reactive. That is one reason some patients develop redness and patches that resemble eczema.
Who Is More Likely to Flare
People with prior eczema, asthma, allergic tendencies, or sensitive skin may flare more easily while taking isotretinoin. Cold weather, long showers, and harsh products can add to that risk.
A person with acne-scar concerns may initially focus on the benefits of acne treatment and miss early signs of barrier damage. When symptoms begin, early skin care changes often matter more than waiting for the rash to worsen.
Soap, Friction, and Hand Washing
Frequent hand washing, strong soap, and repeated friction can push dry skin into a more inflamed state. This is common on the backs of the hands, around the knuckles, and near small cracks in the skin.
Even routine tasks like cleaning, typing, or using sanitizer can make symptoms worse. Gloves for wet work and gentler cleansers may help limit extra irritation.
Sun, Weather, and Other Triggers
Many patients on isotretinoin become more sensitive to the sun, and excessive sun exposure can add redness and discomfort to already dry skin. Wind, low humidity, and indoor heat can also increase water loss from the skin.
Some people notice worse symptoms after exercise, travel, or long days outside. These triggers do not cause eczema by themselves, but they can make a weak barrier flare more easily.
Accutane Rash vs Eczema
Some patients benefit from a broader overview of how dermatologists evaluate different types of rash when the cause is not obvious. Some patients have simple dryness, others develop retinoid dermatitis, and others have new or worsening eczema.
The pattern, texture, itch level, and location often give useful clues. A careful history and skin exam are sometimes needed when the diagnosis is not clear.
Signs of Irritation and Xerosis
Xerosis refers to very dry skin and is one of the most common side effects of isotretinoin. It often causes roughness, scaling, mild redness, and a tight feeling after washing. The rash may burn more than it itches, and it often appears in areas already prone to dryness.
This pattern is usually broader and less sharply inflamed than classic eczema.
When It May Be Eczema
Eczema often causes stronger itching, patchy inflammation, and repeated flares in the same areas. The skin may look red, cracked, thickened, or flaky, and scratching can make it worse. In some cases, the rash starts after Accutane but presents like eczema because the skin barrier is already compromised.
That is why Accutane and eczema can be linked in practice even when the medication is not the sole cause.
When It May Be Retinoid Dermatitis
Retinoid dermatitis is a form of irritation related to the effects of vitamin A–based treatments on the skin barrier. It can look similar to eczema, but it often tracks closely with dose changes, harsh products, or overcleansing.
The skin may sting, peel, and react quickly after contact with soaps or active ingredients. A clinician may need to determine whether the rash is simple irritation, eczema, or another inflammatory condition.
Accutane Eczema Hands and Other Flares
Hand symptoms are common because the hands are exposed to repeated washing, friction, and weather exposure every day. Patients may search for Accutane eczema on the hands when the skin becomes red, cracked, or painful during normal activities.
This area often flares first because it gets less natural oil and more outside stress than many other body sites. Foot blisters or coin-shaped patches can also occur, though they are less common.
Accutane and Dyshidrotic Eczema
Accutane and dyshidrotic eczema may overlap when small, itchy blisters appear on the sides of the fingers or palms. This pattern differs from plain dry skin, as it often includes deeper bumps and intense itching. Sweating, stress, and repeated exposure to water can make it worse. A dermatologist may need to confirm the diagnosis if blistering is present.
Other Eczema Patterns Reported
Some patients report round, scaly patches that resemble nummular eczema, while others notice broader, dry, itchy areas on the arms or trunk.
These patterns are not the most common, but they are among the skin changes seen during isotretinoin therapy. That is why history, location, and timing all matter. A single label does not fit every rash that appears on Accutane.
How to Deal with Accutane Rashes and Eczema
How to deal with Accutane rashes and eczema depends on the severity of the symptoms and whether the problem is primarily dryness, clear eczema, or another form of dermatitis. The first step is often to protect the barrier with bland products and reduce avoidable triggers.
Prescription treatment may be needed when the skin becomes very inflamed, painful, or hard to manage at home. Care should remain simple, as too many products can increase skin irritation.
Accutane Eczema Treatment Basics
Accutane eczema treatment often starts with thick fragrance-free moisturizers, gentle cleansing, and avoiding exfoliants or drying agents. Some patients also need a short course of prescription anti-inflammatory treatment from their dermatologist.
The goal is to calm inflammation while protecting the skin barrier. This does not replace acne treatment planning, but it helps reduce the burden of potential side effects.
What Is the 3-Minute Rule for Eczema?
The 3-minute rule means applying moisturizer within about three minutes after bathing or washing, while the skin is still slightly damp. This helps trap water in the outermost layer of skin before it evaporates. It is a simple method, but it can make daily moisturizing more effective.
For patients on isotretinoin, this step often works best when paired with short lukewarm showers and mild cleansers.
Moisturizers, Cleansers, and Hand Care
Choose thick creams or ointments over light lotions when the skin is very dry or cracked. Use a gentle cleanser once or twice daily, then follow with moisturizer and lip balm as needed.
For hands, reapply cream after washing and wear protective gloves for cleaning or dishwashing. In a medically focused DermOnDemand article like this one, these steps matter because simple, routine changes often prevent further deterioration.
Does Eczema From Accutane Go Away?
Many cases improve after the drug is stopped or the skincare routine is adjusted, but the timeline varies. Some people recover quickly once dryness settles, while others need longer care if eczema was present before treatment.
Does eczema from Accutane go away is a reasonable question, yet the answer depends on the cause of the rash and the person’s baseline skin health. Persistent symptoms should not be dismissed as normal if they continue to spread or interfere with daily life.
Will Eczema Go Away After Stopping Accutane?
Will eczema go away after stopping Accutane is a common follow-up question, and in many patients, the skin improves once oil production starts to normalize. Still, recovery is not always immediate because the barrier needs time to rebuild. People with underlying eczema may continue to flare even after isotretinoin ends. That is one reason ongoing follow-up can be useful when symptoms do not settle.
Can Accutane Cause Permanent Eczema?
There is no simple rule that Accutane causes permanent eczema in most patients. More often, it causes dryness and irritation that can uncover or worsen a tendency the person already had. Some patients remember the flare as beginning with the medication, but that does not prove permanent damage.
A long-lasting rash warrants a proper review because eczema, dermatitis, infections, and other skin conditions can look similar.
When to Contact a Dermatologist

Contact your dermatologist if the rash becomes very painful, widespread, blistering, or infected, or if home skin care is not helping. If symptoms are progressing and you need the next steps, you can start treatment after deciding that direct dermatology review is appropriate. Crusting, pus, bleeding, fever, or severe swelling can indicate a problem that requires direct medical care.
Patients who are sensitive to the sun may also need advice if sun exposure is making inflammation harder to control. It is better to ask early than to keep layering on products that may worsen the skin.
Warning Signs That Need Review
If deep cracks, severe itching, a painful hand rash, or a sudden worsening start to interfere with sleep or daily tasks, it is time to seek medical guidance. Rash near the eyes, signs of infection, or extensive peeling should not be ignored, as these changes may indicate that your skin barrier is too inflamed for routine home care alone.